Overview | Causes | Symptoms | Diagnosis | Treatment | FAQ
Overview
Adult Kyphosis | Adolescent Kyphosis
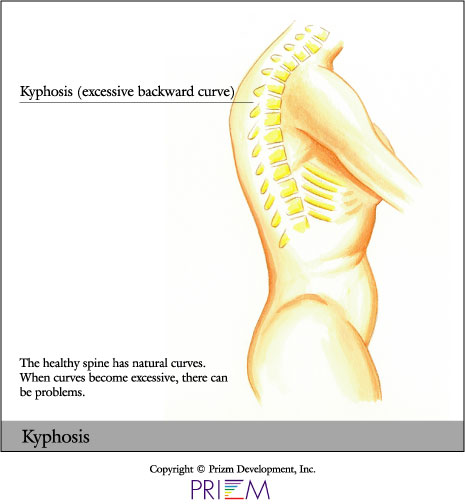 Kyphosis and lordosis are types of spinal deformities. While
slight curvature of the spine is normal and healthy, there are some
cases where it is over-pronounced and can cause both cosmetic deformity
and health risks. Lordosis occurs when the spine curves too far inward in the low back. Kyphosis occurs when the spine in the shoulder blade area curves forward more than normal. Individuals with kyphosis may have visible humps in their back. Kyphosis or Scheuermann’s disease most often occurs in the thoracic area
of the spine and is often noticed as adolescent roundback or stooping.
Kyphosis and lordosis are types of spinal deformities. While
slight curvature of the spine is normal and healthy, there are some
cases where it is over-pronounced and can cause both cosmetic deformity
and health risks. Lordosis occurs when the spine curves too far inward in the low back. Kyphosis occurs when the spine in the shoulder blade area curves forward more than normal. Individuals with kyphosis may have visible humps in their back. Kyphosis or Scheuermann’s disease most often occurs in the thoracic area
of the spine and is often noticed as adolescent roundback or stooping.
A normal kyphosis curvature is 40 degrees in young adults. Curves over 70 degrees are often associated with more lifelong pain and may result in a more sedentary profession than normal patients.
Causes
Some people are born with kyphosis when there is a naturally occurring abnormality in the spine. Kyphosis can also be an acquired condition. Teenagers in particular may develop kyphosis due to bad posture, especially girls between the ages of 12 and 15. Adolescent and adult kyphosis is called Scheuermann's disease.
Compression fractures are often linked to the development of many cases of adult kyphosis, because they cause vertebrae to become wedged, reducing the amount of space between each vertebra. These fractures can occur as the result of degenerating discs, arthritis, osteoporosis and spondylolisthesis. Individuals with osteoporosis may develop kyphosis due to a weakening and compression in the vertebrae. Kyphosis in these individuals is treated with aggressive anti-osteoporosis action to prevent further bone weakening.
Other causes may include previous lumbar surgery with fusion for back pain, scoliosis or stenosis. This lumbar fusion may lead to “flatback” or permanent stooping. In these patients spinal balance issues can go unnoticed and a flatback result. A previous failed surgery on the spine may also lead to kyphosis.
Symptoms
The symptoms of kyphosis are similar to those of scoliosis. These include
uneven shoulders, chest, hips, shoulder blades, waist, or a tendency
to lean to one side. In other cases, there are no visible symptoms.
To diagnose a person with scoliosis, have them touch their toes.
If either one or both shoulder blades are prominent, the waist is
shifted or ribs are uneven, kyphosis may be present. Kyphosis is
also called “hunchback” because of the hunched over appearance
often seen in patients. Other symptoms include fatigue and difficulty
breathing.
Diagnosis
Outlined below are some of the diagnostic tools that your physician may use to gain insight into your condition and determine the best treatment plan for your condition.
- Medical history: Conducting a detailed medical history helps the doctor better understand the possible causes of your back and neck pain which can help outline the most appropriate treatment.
- Physical exam: During the physical exam, your physician will try to pinpoint the source of pain. Simple tests for flexibility and muscle strength may also be conducted.
- X-rays are usually the first step in diagnostic testing methods. X-rays show bones and the space between bones. They are of limited value, however, since they do not show muscles and ligaments.
- MRI (magnetic resonance imaging) uses a magnetic field and radio waves to generate highly detailed pictures of the inside of your body. Since X-rays only show bones, MRIs are needed to visualize soft tissues like discs in the spine. This type of imaging is very safe and usually pain-free.
- CT scan/myelogram: A CT scan is similar to an MRI in that it provides diagnostic information about the internal structures of the spine. A myelogram is used to diagnose a bulging disc, tumor, or changes in the bones surrounding the spinal cord or nerves. A local anesthetic is injected into the low back to numb the area. A lumbar puncture (spinal tap) is then performed. A dye is injected into the spinal canal to reveal where problems lie.
- Electrodiagnostics: Electrical testing of the nerves and spinal cord may be performed as part of a diagnostic workup. These tests, called electromyography (EMG) or somato sensory evoked potentials (SSEP), assist your doctor in understanding how your nerves or spinal cord are affected by your condition.
- Bone scan: Bone imaging is used to detect infection, malignancy, fractures and arthritis in any part of the skeleton. Bone scans are also used for finding lesions for biopsy or excision.
- Discography is used to determine the internal structure of a disc. It is performed by using a local anesthetic and injecting a dye into the disc under X-ray guidance. An X-ray and CT scan are performed to view the disc composition to determine if its structure is normal or abnormal. In addition to the disc appearance, your doctor will note any pain associated with this injection. The benefit of a discogram is that it enables the physician to confirm the disc level that is causing your pain. This ensures that surgery will be more successful and reduces the risk of operating on the wrong disc.
- Injections: Pain-relieving injections can relieve back pain and give the physician important information about your problem, as well as provide a bridge therapy.
Treatment
When treating kyphosis, the cause of the disease must first be considered.
Some cases require surgery early on, while other times, bracing and
physical therapy may be the best course of action. Although bracing
can help reduce pain symptoms, it is less successful at fixing the
underlying problem of a curved spine, especially in adults. Bracing can be used for progressing curve in skeletally immature patients. Strengthening
and stretching programs can be successful at reducing symptoms. Swimming
and other low-impact forms of exercise are beneficial. In cases which
require surgical intervention, such as a large or progressive deformity, the goal is to reduce the curvature
and relieve pain and discomfort over a long period of time.
[Top]
The common type of surgery for kyphosis used to be a large anterior and posterior surgery. Today, the condition may be treated with a less invasive posterior-only Ponte procedure,
Scheuermann's Disease in Adolescents and Adults
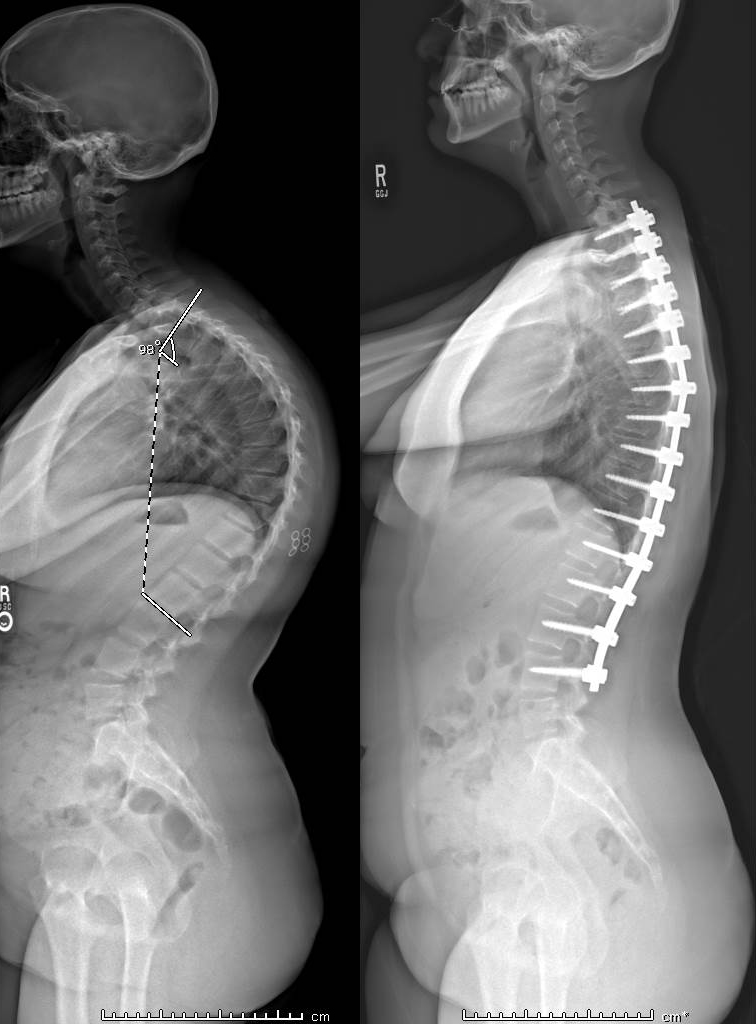 Scheuermann's kyphosis, manifesting in a “roundback” or “hunch” deformity, is a developmental type of kyphosis occurring while the body is still growing. Normal vertebrae are rectangular shaped and stacked on top of one another like building blocks with a soft cushion disc between each one. When Scheuermann's kyphosis occurs, the front of the vertebrae wedge forward and closer together in a triangular shape. This causes the spine or curve to move forward and closer together in a triangular shape and the spine to curve forward more than normal.
Scheuermann's kyphosis, manifesting in a “roundback” or “hunch” deformity, is a developmental type of kyphosis occurring while the body is still growing. Normal vertebrae are rectangular shaped and stacked on top of one another like building blocks with a soft cushion disc between each one. When Scheuermann's kyphosis occurs, the front of the vertebrae wedge forward and closer together in a triangular shape. This causes the spine or curve to move forward and closer together in a triangular shape and the spine to curve forward more than normal.
Scheuermann's kyphosis develops in adolescents while their bones are still growing. It happens to about 0.1% percent of people in this age group and occurs a little more often in boys as girls.
This kyphosis, or roundback, can lead in larger curves to difficult spinal deformities and pain. Initial treatments, depending on the age of the patient, residual growth, and size of curve, can include physical therapy, bracing, or injections. In larger or progressive curves resistant to conservative treatment, surgery is an option. This can be done minimally invasively via a dual VATS/percuateous approach, or a single approach Ponte procedure.
In adults in whom Scheuermann's kyphosis is untreated, it can be a cause of progressive roundback, pain, and overall spinal imbalance.
Click here to learn more about Scheurmann's Disease
Global and Focal Kyphosis
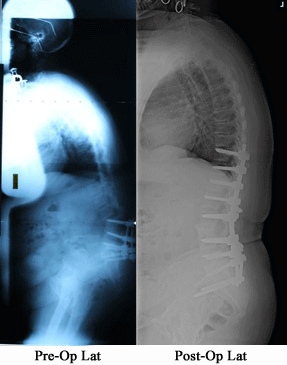
Adult Kyphosis, either stooping (global kyphosis) or roundback (focal kyphosis) can be caused be multiple factors. This can range from a Scheuermann's kyphosis or adolescent roundback that was never treated to the previously operated spine or scoliosis (flatback). In rare cases, previous fractures, congenital anomalies, inflammatory disorders, or neurologic disorders may play a role.
In adults, the risks of kyphosis surgeries can be significant. Initial treatment is focused on the symptoms of the kyphosis and is usually conservative. In the case of progressive disability, pain, and deformity, surgery may be helpful if the benefits outweigh the risks.
Click here to learn more about Adult Kyphosis
FAQs
When is surgery necessary to treat kyphosis?
Surgery is always treated as a last resort, while more conservative methods are tried first. In general, surgery is considered when the curve exceeds 75 degrees. Other cases in which surgery may be recommended are for those suffering from chronic pain and/or a rapidly progressive curve.
How can I prevent kyphosis?
Strengthening the back muscles can help prevent poor posture, which
can lead to kyphosis. Osteoporosis, which can also cause kyphosis,
can be prevented by getting enough calcium and vitamin D, exercising
and strength training regularly.